This article looks to be a reasonably comprehensive assessment of a disease that is varied and under-reported and annoying (i know from experience). Establishing facts and organizing data is about all we can do.
My goal is to try to figure out what the mechanism is so that I can contribute to an appropriate treatment option (selfishly for myself but hopefully benefiting others). An update on the food sorting and avoidance, I figured that after three or four weeks of not eating some foods, that if i did not see an improvement, yet even saw increase numbers of lesions that “food” was the least of my worries. But, that said, I am certainly increasing by volumes the amount of vitamin A that i am ingesting through natural sources…which leads me to recommend sweet potatoes, and red bell peppers, some dairy, since these foods have reasonable amounts of vitamin A. I am not inclined to eat organ meat, i could try fish oil.
Here is a tiny tidbit of data: When i had three biopsies (shoulder, leg, and dorsal forearm, a bandaid was put on each, and while NO lichen planus lesions grew in the biopsies…haha… they did appear under the tape marks of the bandaid. Now when Dr. Blabla says there is NO ENVIRONMENTAL component… they are just wrong.
That lesions are bilateral, mmm possibly, in my case it seems right side shins are worse than left… but so were the initial lesions created by my lawnmower (those pesky rocks, sticks, and shards of acorn) thrown back into my shins — the origin of the large lesions, and the only place that I have lesions larger than about 7-8mm diameter. Half a dozen of those on my shins are 20-30mm in diameter and 5-7mm thick. I think it is hypertrophic vesiculobullous lichen planus… two in one — LOL. I can confirm that the worst lesions are on “sun-exposed” areas of legs and arms.
This review (linked) above unfortunately does not do a good job of explaining all the nuances of the pathological architecture, structure, or ultrastructure and parrots what has been published in countless other places… though i suppose this is due in part not having a truly committed pathologist. I have tried but have not been successful (even though promised by the MD) to have access to the slides to read them myself.
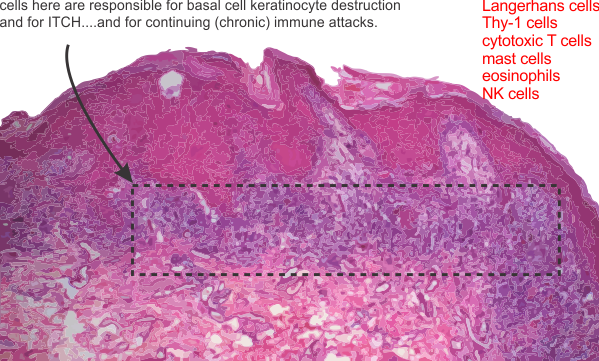
When i read the slides i will take careful count of the mast cells, eosinophils and basal keratinocyte destruction to figure out if this (my case) is a lichenoid drug/chemical (in my case would be chemical) reaction rather than classical cutaneous lichen planus.
In retrospect, those who name the disease for the look of “lilchen” on the barks of trees sort of did the whole deal a disservice. And while they did not know the cause, and the cause is not known today, might have been smart not to name the disease after something that grows on tree bark. ha ha
The list of drugs which cause lichen planus like lesions is long and the number of drugs on the list given in this report would include something taken by almost everyone, and includes simple things like ibuprophen. good grief.
One thing that keeps coming to mind is perhaps a mixed-cause… that underlying condition possibly left over from a shingles outbreak, or a viral infection, or maybe even a series of bug bites that stimulate some immune response that is triggered to go into overdrive by an environmental exposure (as in my case, perhaps related to mortar, cement and ground exposure over a 10 year period). Would that someone in this insitution (there are those, like the Berensteins here in the department that are in tune to environmentally and occupationally triggered diseases, but they were too busy to take note. Just to belabor the point, the university of cincinnati does NOT take care of its own. One would think that being 50 years at this institution that I could call upon one of the MDs, (someone in the same department of environmental health, as i am, like the Bernsteins) and expect some kind of compassionate treatment…or to be able to email the pathologist who was supposed to have looked at the histological preps, Dr. Mutasim) but no such luck, in fact quite the opposite — how sad). NO perks for having spent 50 years doing research here.
Paper listed above does regard many metals as possible factors in LP reaction…so if the metals can trigger this in crowns and fillings, why not also metals found in other occupations, e.g. cement, mortar, grout, tile and similar applications. Still i could not get the attending MD in my case to do anything but scoff at the idea.