Well, that was slightly disappointing. Looking for, at most 6 minutes, through three slides was less than uplifting. The classic look: mild hyperkeratosis (thickening of the stratum corneum, or that uppermost layer of skin cells (which are without nuclei) and usually includes some additional keratin; infiltrate and apoptotic basal keratincytes; and acantholysis (the loss of intercellular connections, such as desmosomes and adhesion molecules (that can cause separation of keratinocytes in the middle and basal layers, and also signal cells to undergo apoptosis) and lots of cell debris and apoptotic bodies in the basal layer of the skin. With this there are numerous infiltrating lymphocytes (which the literature calls Th-1 cells) that apparently are able to send self destruct messages to the basal keratincytes. All this was surely evident in the slides (3 separate biopsies) from my own case of lichen planus. That said…. you ask, why are you disappointed?
Disappointed in the lack of “interest” in the real histology..like actually viewing at a magnification worth looking at… ha ha…. for an electron microscopist to be satisfied looking at 10, 40 or 60X H&E is like asking the driver of a Koenigsegg Agera RS to be happy on a scooter. While I recognize acutely (bad pun for a chronic dermatosis) how difficult it is to get through a day of reading slides I just didn’t get the feeling of thoroughness from this man, and also got a definite thumbs down when I suggested that there might be an environmental component. What gives? do the old MDs think that all of life grew up in a space-vacuum… the environment is critical.
Another question that I asked and was surprised at the answer was whether there was a good database for lichen planus cases…. he asked “database” So i asked again, to see if there were a lot of cases….so apparently there are not.
Online publications seem to suggest that lichen planus (i assume they include all variations) is 1-5% of the population? To me… that would be a lot.
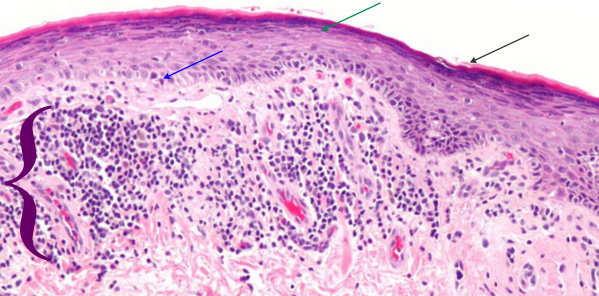
Here is a picture (wikimedia commons) which is a lot like (not exactly) what my slides showed. Blue arrow points to keratinocytes which are undergoing apoptosis (sometimes by the old guys called Civatte bodies), green-blue arrow points to area of stratum corneum, and black arrow to the keratin layer. White space is separation of intercellular junctions and are part of the disease process. Purple bracket = the band of infiltrating cells (for all practical purposes at this low magnification… one has to just call them mononuclear cells (which would include most cell types… ha ha). Bright pink rounded areas in dermis are blood vessels.
When i asked about langerhans cells, Thy-1 cells, melanocytes, that just drew a “no comment look” for obvious reasons, the magnification was too low, as was the interest in finding something out about these participating cells and the extent to which they might be found in different numbers in cases with different origins. While I dont discredit the authenticity of the diagnosis from the pathologist i met with today, I do feel that the barest minimum of reporting was made, with great emphasis on “i need to move on to read other slides” and “dont bother me lady”. This is part and parcel for being an old lady in science. It is ok to be an old male in science…. but the gender bias is alive and well.
THere was also no interest expressed in doing anything in the way of a study about the variety of immune cells, their possible connection with cumulative, and concurrent environmental triggers. Ok, that makes me pretty energized to figure this out some other way…the pathologists here are not going to be of much help.
I have three new ideas:
I) the disruption of adhesion molecules (that would be dozens of molecules which comprise portions of the desmosomal, adherens and tight junctions, of which many participate in cell signaling i.e. apoptosis. The adjesion molecules may be a direct or indirect response so that I will have to google.
2) The apoptotic cells: are these self induced apoptoses due to loss of adhesion molecules, or are these apoptoses achieved through the infiltration of Th-1 cells (cytotoxic T-lymphocytes (CD8+) and NK (“educated”by langerhans cells) which have as their goal to annihilate basal keratinocytes. A few ways to kill basal keratinocytes –by the release of perforin and granzyme or by the Fas/FasL system.
3) Are mast cells and eosinophils involved, particularly in the release of vasoactive substances, upon touching, sheering or stretching the lesions, which then triggers enormous itching.
4) another question would be, if this is indeed a “educated” set of Th-1 and NK cells, how long would one suppose that the “commitment” of those cells last. Would it be a life long immunity gained, or something that passes quickly.
